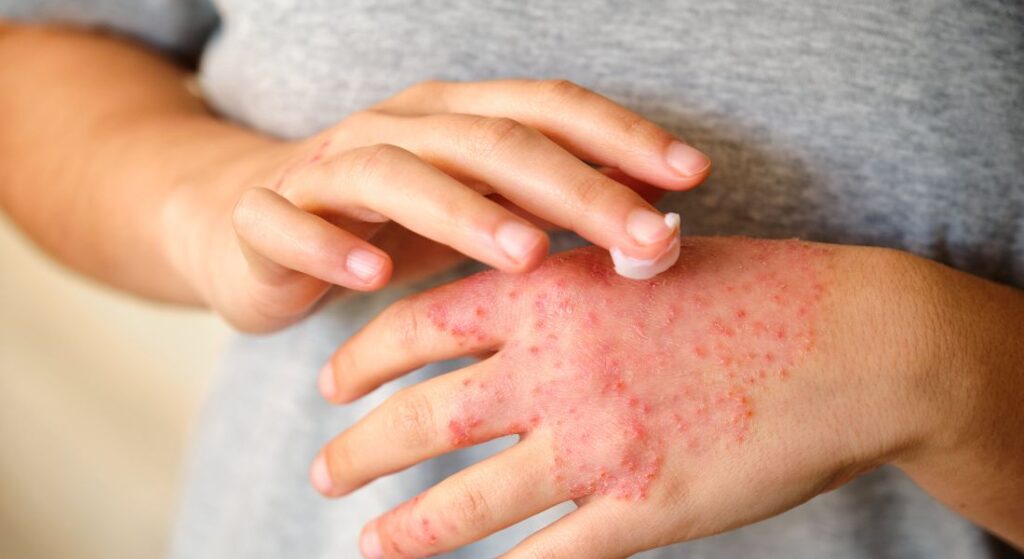
One thing that is a tough pill for all of us to swallow is the concept of “chronic” in health care. No one wants to hear that something is long-term, fraught with ups and downs and not just a one-time deal that can be cured with a short course of antibiotics. But who wants to be on medication for the rest of their life? Well, if you have a skin condition like psoriasis, atopic dermatitis or hidradenitis suppurativa that prevent you from living your best life, you probably would be willing to make that decision. We are just fortunate that now we have excellent therapeutics to do just that and more in the pipeline.
What’s interesting is that with medication, chronic does not mean debilitating and often you might even forget that you have a diagnosis. Take blood pressure for example. I can’t tell you how many times a patient has forgotten they have high blood pressure, yet they are on a beta blocker for it. When I inquire more, the response is usually, “I don’t have high blood pressure but yes I take medicine for it.” It’s fascinating that the control the medication offers conveys a sense of cure, rather than control. When I offer an alternative explanation of, “Yes, the medicine puts your blood pressure back into a healthy range, but technically you still have high blood pressure,” my words are often met with a confused look. On the bright side, it shows how powerful control is.
When describing skin conditions like atopic dermatitis (AD), psoriasis and hidradenitis suppurativa, I always set expectations with what I call the three C’s—Its’ Chronic, We can’t Cure it but we can Control it. Most patients get the message—this is one of those annoying things that I am not going to eliminate from your health history, but I am going to create a treatment plan that offers tight control. But I also want patients to understand that flares can happen, or what I call blips on the radar. As long as these calm down, aren’t too frequent and you quickly go back to a controlled baseline, then that’s a part of chronicity. We can always control for every trigger, like stress or infection, even with the best therapies. The goal is to make those blips as rare as possible and now we have medications that can potentially accomplish just that.
Remission definitions can be on or off therapy. While we are waiting for a consensus with atopic dermatitis, there is a consensus for psoriasis on therapy. The Remission Workgroup of the National Psoriasis Foundation (NPF) defined on-treatment remission for plaque psoriasis as patients maintaining a body surface area (BSA) involvement of 0% or an investigator’s global assessment (IGA) of 0 for at least 6 months. The off-treatment remission for plaque psoriasis is defined as maintaining a 0% BSA without any treatment for at least 12 months. The challenges are can everyone meet this criteria and is it still acceptable for minor flares or blips? Will new drugs or regimens be able to satisfy this definition or be required to have a certain number of patients reach remission in order to be approved? Will patients want to drug or biologic hop more often if they do not achieve remission, maybe they only got 5 months before they had a minor flare due to stress? And if you thought insurance companies didn’t care about remission, then you’re wrong. Payers also think remission definitions are important for long-term coverage of medications. That’s a different perspective that might come with its own challenges.
Overall, the concept of remission is simply fascinating. When I talk about it with my patients, one of them told me, “Great, doc, So I’m cured like if I had cancer?” And then I realized one of the pitfalls of remission from a patient’s perspective. There’s always two sides to the coin of what we understand as healthcare providers and what our message conveys to patients. Remission is a powerful concept but we should be careful to let patients know that it can also be complex because of the dynamic nature of the immune system, it does not mean the same thing as a cure and there are agreed definitions of what remission really is. What’s more is remission can also play a role with compliance and influence a patient’s choice to stop a medication suddenly. We already see this with some biologics that have remittive effects, often observed because patients have voluntarily stopped their medication and noticed a period of control before inevitably, their AD or psoriasis returns. In the end, remission conversations will require expectations check so that both the provider and patient are on the same page.
Trotter’s Take: Remission for chronic inflammatory disease is an exciting reality that we are ready to embrace in dermatology..
Do you think remission is possible? Then you need to listen to Dr. Joe Tung as he talks more about remission in psoriasis and eczema and where the future is headed.